Procedures
Knee preservation: Subchondroplasty (SCP) procedure
Age is just a number. We all strive to lead a full and active life. It doesn’t matter if it’s for work, sports, leisure or caring for our loved ones. Knee pain does creep up on us every now and again and spoilt these plans. Sometimes it’s related to strenuous activities and gets better with time and rest. Other times it lingers for longer than we would like and starts to affect our basic daily activities like walking up the stairs, running after the bus or even get a good night’s sleep.
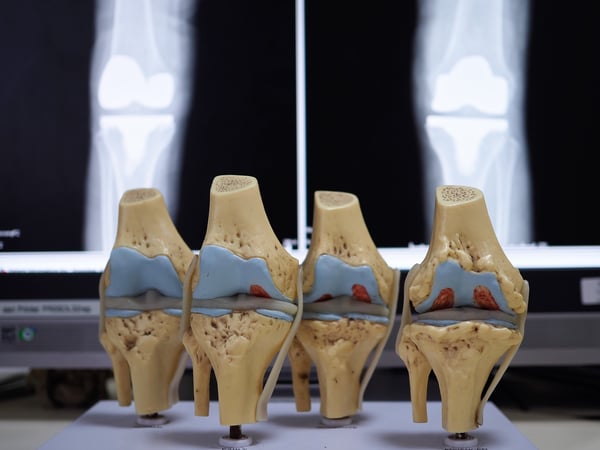
I often see patients between the ages of 45 and 75 years old who fall in this category. They have very localised or specific knee pain that really hampers their daily function. This is despite them having a good body weight, wearing good supportive shoes and not over straining. While x-rays of their knees look almost normal, their MRI scans paint a different picture. Their MRI scans often report mild arthritis of their knee with some degeneration of their meniscus. What strikes me most is the bone swelling or oedema that often shows up on their femur, tibia or both. These areas of bone oedema are known as bone marrow lesions (BML).
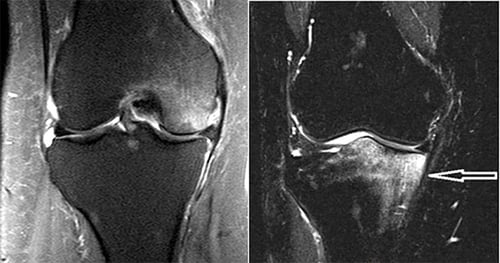
We used to think that bone oedema was a reflection of stress forces in that area. There is now evidence to show that that bone oedema actually reflects bone that is mechanically and histologically altered. These lesions are associated with pain, bone deformation and accelerated osteoarthritis progression. Under the microscope (histologically), these lesions show evidence of fibrosis, fat necrosis (death), micro-fractures of the trabecular bone and poor mineralisation. All these factors confirm that the bone in this area is not able to form with normal characteristics. Patients with such BMLs are reportedly 9 times more likely to undergo a total knee replacement within three years.
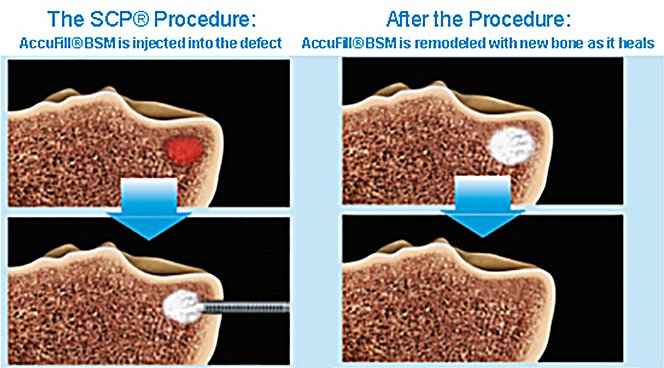
We now act pre-emptively when we spot these BMLs. Knee preservation techniques such as meniscal repairs have long been done. Subchondroplasty (SCP) is a minimally invasive technique to apply a synthetic bone substitute (calcium phosphate-based) into the BMLs to reduce pain, improve function and delay the need for a knee replacement in the following years. The aim of this procedure is to improve the structural quality of the affected subchondral (area of bone just below the cartilage) bone, promote local bone remodelling to prevent bone collapse and progression of arthritis. Calcium phosphate has long been used in orthopaedic surgery to overcome bone defects in a spectrum of cases such as trauma, tumour and adult reconstruction. It remodels and is replaced by patients’ own bone after several months.
The procedure involves small incisions in the skin around the knee where cannulas (instruments smaller than chopsticks) are inserted. Fluoroscopy (intra-operative X-rays) are used during the surgery to ensure the cannulas are in the right position. The cannula is then advanced into the BMLs themselves. The bone substitute in the form of a paste is prepared and injected through the cannula into the middle of the BMLs. With fluoroscopy we can ensure that all of the bone substitute pate is applied accurately into the BLS and not into the knee joint. The bone substitute hardens fully within about 10 minutes, allowing patients to full weight bear immediately. Patients may go home on the same with simple analgesia as required. If there are other degenerative injuries in the knee such as a meniscus tear, I will address these lesions at the same sitting arthroscopically (keyhole technique). Your rehab protocol will therefore be a little different if this happens. Published data has shown significant improvement in knee pain within a week of this subchondroplasty procedure and is a safe new treatment modality for early stage osteoarthritis when an associated bone marrow lesion is present.
Is it alright to walk around with a sprained ankle?
This depends on the sprain's severity and what treatment has been rendered for the injury. Your doctor may advise you to only put minimal weight on your ankle while it is still recovering from the injury. Excessive walking may lead to more pain and swelling if the injury is stressed too early on.
How do I know if my ankle sprain is serious?
The nature of the initial accident or injury will provide a good idea about how fast it may recover. A serious injury is characterized by severe pain, swelling, and recurrent sprains despite efforts to support and treat it. If you are experiencing these, the soonest visit to the specialist is highly advised.
Can I claim insurance for my ankle injury?
Ankle sprains and injuries are insurance claimable. We do advise our patients to check with their personal or corporate insurance plans and representatives. We are also able to help them with this if required.
What should I do immediately after an ankle sprain while waiting for my appointment and treatment?
Timely self-care with rest, icing, compression, and elevation are important to manage the initial pain and swelling around the ankle. Anti-inflammatory medication will further reduce the pain and swelling that you may be experiencing.
I have more questions, how can I speak to a doctor?
Please call us at +65 6733 4565 (during office hours), or drop us a text or WhatsApp message at +65 9766 4565. We will reply to your queries as soon as we get them. You may also call to make an appointment to see Dr. Mizan for your ankle injury.